On Evidence so Far Vaccines Temporarily Ramp Up Antibodies but Do Not Build Underlying Long-Lasting Immunity
Does not leave the body with the ability to recognize the virus the way infection does

The latest data from Israel and the UK on covid vaccine effectiveness.
The latest data from Israel, which has used primarily the Pfizer mRNA vaccine, indicates that vaccine effectiveness against Delta coronavirus infection and symptomatic (“mild”) disease has dropped from about 95% to about 40%, whereas effectiveness against hospitalization and severe disease (i.e. low blood oxygen levels) remains at 80% to 90%.
Importantly, in people who got vaccinated already in January 2021 (primarily the elderly), protection against infection and mild disease may already have dropped to near 0%. Moreover, since the Delta covid outbreak is still accelerating in Israel, the effectiveness against hospitalization and severe disease may further decrease (due to lags in hospitalizations).
(Update: New data from Hebrew University shows that protection against severe disease has already dropped to 80%; compared to the original 96%, this results in a five-fold increase in residual risk.)
In the UK, which has primarily used the AstraZeneca DNA adenovector vaccine, the latest estimate by researchers at University College London indicates an effectiveness against infection of about 20% and a total effectiveness against severe disease of about 60%. In very senior citizens, the effectiveness against severe disease may be even lower (due to a weaker immune response).
(A substantially higher estimate by Public Health England, recently published in the New England Journal of Medicine, was based on outdated data from early June. Interestingly, the British government hasn’t updated its data on AstraZeneca vaccine effectiveness since June 13. Update: New data from PHE confirms that effectiveness against infection has dropped below 20%.)
The Israeli data shown above indicates that effectiveness against infection and mild symptoms decreases rapidly over time and reaches near-zero levels after about half a year. Most likely, this is because covid vaccines do not achieve mucosal immunity (in contrast to natural infection) and serum antibody levels (i.e. antibodies in the blood) decrease within months.
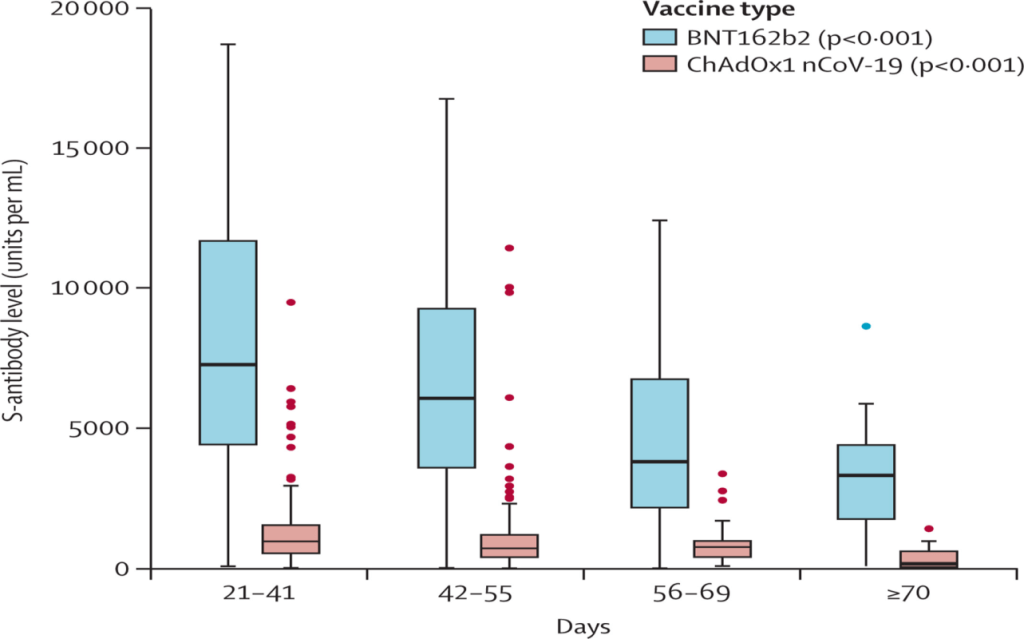
Thus, the false promise of very high protection against “symptomatic infection”, found during official vaccine trials, was simply based on very high short-term serum antibody levels mimicking mucosal immunity. Conceivably, the pharmaceutical companies may even have known that this was just a (very lucrative) “flash in the pan” and not a lasting protective effect.
In contrast, protection against severe disease is achieved by lower serum antibody levels in combination with immunological memory (B cells) and cellular immunity (T cells). However, the Delta variant has already achieved partial immune evasion (as did Beta and Gamma, but not Alpha), and future coronavirus variants will likely achieve almost complete immune evasion.
Thus, vaccine protection even against severe disease will likely further decrease due to new variants, or, in the very worst case, will turn into antibody-dependent disease enhancement (ADE), if high levels of non-neutralizing antibodies aggravate the infection. Indeed, this is what happened in the case of vaccines against SARS-1 and dengue fever.
To prevent such a decrease in protection against severe disease, or to restore short-term protection against infection and mild disease, updated “booster shots” will likely become necessary. (Update: On July 29, Israel announced “booster shots” for people over 60 years of age.)
However, there is a very real risk that additional vaccinations, which inject or induce the coronavirus spike protein, could substantially increase the risk of serious cardiovascular and neurological adverse events, such as strokes, GBS and heart muscle inflammation. Globally, covid vaccines may already have killed tens of thousands of people. Alternatives include safer oral vaccine candidates or medically supervised, low-dose oral live virus challenges in low-risk people.
Furthermore, the millions of people who were told that vaccination will protect them against a coronavirus infection will soon have to realize (once again) that this is not the case: instead, most of them will get infected anyway. On the positive side, this may actually provide additional mucosal immunity to large parts of the population while being mostly protected against severe disease.
Indeed, data from Israel as well as recent studies all indicate that a previous coronavirus infection continues to offer the best protection against future infections and disease.
In contrast, vaccination cannot achieve “sterile immunity” against infection and infectiousness. Thus, the whole idea of “vaccination certificates” has become obsolete – at least from a medical and epidemiological perspective – and should be rejected: the claim that it’s just “the unvaccinated” that are driving outbreaks – a claim made by many authorities – is simply false.
For instance, just this week a “fully vaccinated” Australian managed to pre-symptomatically infect about 60 people at a party in the United States. Many similar stories have already been reported in Europe and Israel: fully vaccinated people can easily transmit the virus even to large groups. Hence, imposing “vaccination certificates” or “green passes” may only serve a political purpose.
(Update: New data from Israel shows that “only 20%” of fully vaccinated people have infected others in public spaces. While authorities claim that this is a success, in reality, it is not any different from unvaccinated people, thus confirming zero effectiveness against infection and transmission.)
In many countries, mass vaccination campaigns have themselves triggered large coronavirus outbreaks (“post-first dose spike”), possibly due to a combination of vaccine-induced temporary immune suppression and infections at large indoor vaccination centers visited by thousands of people. The vaccine-induced temporary immune suppression may also explain the frequently observed post-vaccination appearance of shingles (i.e. herpes zoster reactivation).
Concerning children, since covid remains mostly asymptomatic or mild in them anyway, and since vaccination cannot prevent infection and infectiousness, the vaccination of children and even of young low-risk adults becomes increasingly difficult to justify, especially given the very real vaccine-associated cardiovascular risks to them (e.g. teen myocarditis and cerebral blood clots).
A look at covid data in places like Israel, the UK and Portugal – which were first in Europe to experience the Delta variant summer wave – confirms that, while infections have skyrocketed, hospitalizations have remained rather low and deaths have remained very low so far. In contrast, in countries with a low vaccination rate – such as India, Russia, as well as many Asian and African countries, Delta covid deaths have reached all-time record levels. [That’s a very strange thing to say. Actually, Russia’s all-time record was during the winter. India’s all-time record was recent but deaths have already collapsed since, besides its “all-time record” was still extremely low compared to heavily vaccinated developed countries.]
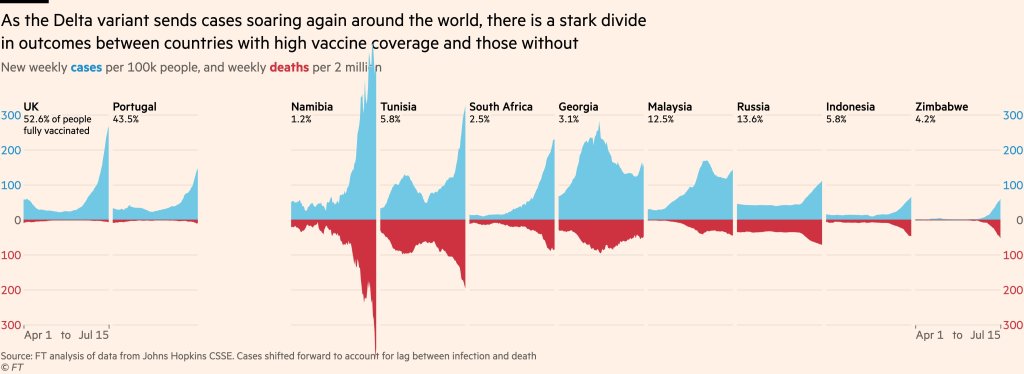
Focus on 'I'
I've decided to compare 3 well-know success-stories (hard LD + vacc.) with a 'failed' India. Added my country Croatia, hope you do not mind.
BTW we have the lowest incidence on Mediterranean, and there still might be some beds available – come and enjoy life! pic.twitter.com/QgnT0vPxJP
— Nenad Bakic (@nbakic) August 2, 2021
In conclusion, and as argued previously, vaccine protection against infection and “mild disease” has pretty much collapsed, whereas protection against severe disease and death remains at a reasonable level, with the partial exception of the most senior citizens and especially nursing home residents, some of whom have never mounted a neutralizing antibody response to the vaccine. Moreover, future coronavirus variants will likely achieve additional immune evasion.
Given the current situation and outlook, it may once again be emphasized that research and implementation of early treatment options for high-risk patients – especially anti-viral, anti-inflammatory (immuno-modulatory) and anti-thrombotic treatment – should be a top priority.
Source: Swiss Policy Research

How are they coming to these results?
What tests are they using to identify COVID, how do we know it is not flu they are testing for?
If they have tests that work…….can we all use them perhaps? I think they are making all this shit up, and it looks like the convenient failure of the vaccines, is an excuse to inject all with ‘Boosters’, just in time for the autumn.
Look how they are now using the ‘alternative media’ to distribute the latest fraud.
I don’t see the article as a fraud . It clearly states the vaccines tested – phyzer and moderna don’t work and shows that the herd immunity is superior, so, one would have to be either stupid or extorted into taking the booster.
Let’s see how many sheep – don’t get the drift and take the big B shot. Stay tuned – the NWO isn’t finished with us yet.
NWO?
You mean the New American order.
I think Kenton is trying to say, that since the CDC is dropping the PCR for a test that ‘can distinguish between the Flu and Covid’ which obviously means the PCR cannot.
Then how could they determine the disease was covid and not the flu?
This seems hard for some to grasp but it appears many have taken the graphene laden injection for a virus that has not been proven to exist.
Who knows what fake test they’ll come up with…. probably another Emergency Use Authorization test like the PCR was.
And yes,,, agreed, mass immunity is far better than any vaccine for any ‘real’ disease.
Your comment verifies my earlier post. It is now common knowledge, that the PCR alleged test, was always a furphy, as made abundantly clear by it’s own inventor. Even after the CDC aknowledge it cannot be used to test for the virus, we still have hundreds and thousands of such test being performed right now, this very minute, and results accepted as Gospel, by Australian ALLEGED health experts and supported whole heartedly by Australian politicians. So how does that go down with the CDC’ latest ruling on this farce ? Apparently the Australian politicians and medical authorities KNOW BETTER, then the inventor of the test and the CDC.
no—the studies suggest effectiveness is of short duration and less than than claimed
So what ??? Is anyone, in any position of authority, or politician taking any notice of such studies and outcomes ??? These people doing the work, may as well flush it all down the toilet, for all the effect it has in the Real World, as should be very apparent by now, anything that does not fit the agenda being persued, is of no consequence. Fulls steam ahead.
“I think they are making all this shit up,…”
Ya think!
I am one of their ‘vulnerable elderly’ and sure as hell don’t want to be vaxxecuted.
Right now I am in the Ok corral and surrounded by the mind controlled Amoeba’s and there is no Wyatt Earp!
Note for the historical purist: The Ok corral thing never happened.
Explain. The OK corral never happened?
The seasonal flu disappears in the summer & will reoccur in the winter.
They have falsely attributed the disappearance of the flu to the vaccine & will now attribute its natural resurgence to a fading of the vaccines strength, requiring boosters. So easily done
Any “vaccines” were never meant to stop COVID. It’s a worldwide eugenics operation.
There is no ‘eugenics operation’, endless ‘treatments’ are now the preferred business model for US big pharma. It is a tax, not genetic engineering.
Dr. Judy Mikovitz jailed for speaking the truth https://www.bitchute.com/video/Y3vny2oca1VL/